The Procedure
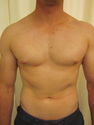
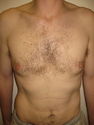
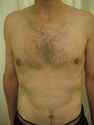
Surgery for gynaecomastia aims to remove the excess breast tissue, fat and skin from the male chest.
There are four grades of gynaecomastia depending on the size of the breast tissue and the amount of skin (Simon Classification).
As part of the pre-operative work up, a full endocrine (hormonal) screen will be employed to ensure there are no underlying causes.
A baseline ultrasound scan will also be performed to ensure it is true gynaecomastia (glandular tissue as opposed to pseudo-gynaecomastia which is adipose or fat tissue) .
An ultrasound scan will clearly delineate and establish the size of the glandular tissue as well as exclude the presence of any suspicious mass within the breast tissue.
Surgery in true gynaecomastia entails liposuction and then removal of the glandular tissue immediately after the liposuction. This is usually reformed through an incision placed from 3 to 9 o’clock at the nipple areolar -skin interface. This produces a faint final scar which is not usually noticeable. The fat under the nipple is also mobilised to prevent any depressions being visible beneath the nipple.
In some circumstances, it may be necessary for skin to be removed.
Surgery is performed under general anaesthetic classically as a day case or with a one night stay in hospital (patient preference).
Drains are usually only placed if an open excision is performed and are left in place for a period of approximately 24 hours.
It is necessary to wear a support garment for a period of six weeks post-operatively.
As part of the surgical work up, a Vectra 3 dimensional computer simulation scanning is produced and this can help patients gain a realistic expectation as to the potential aesthetic result of surgery.
Liposuction and open excision
If glandular tissue is present then this will require an open excision to ensure it’s complete removal.
Liposuction alone (pseudogynaecomastia)
In cases where there is pseudo gynaecomastia, then liposuction alone may be adequate to remove the excess adipose tissue.

Complications and Risks
All Procedures have potential complications and risks. These can be divided into general complications and those specific to each procedure. The latter are listed in the FAQs below.
General complications include:
- Wound complications - bleeding, bruising, collections under the skin of blood (haematoma), pus (abscess), serous fluid (seroma), infection, wound breakdown, suture extrusion, sensory loss;
- Aesthetic complications - poor scars, stretched scars, raised scars (keloid or hypertrophic), contour irregularities, need for revisional procedure;
- Anaesthetic complications
FAQs
-
What does the surgery involve?
If the excess is mainly due to excess fat, a reduction is possible with liposuction alone. This technique relies on good skin tone to contract and take up the excess once the fat is removed.
Dense fibrous tissue may require an open procedure. These techniques can be discussed with Dr. Belt personally.In cases where a patient has lost significant weight or has had a large volume of adipose (fatty) tissue and / or breast gland removed, then some skin may require removal. This can either be performed as a 2 stage operation or as a single procedure. The final scar may be a (semi) circular scar around the nipple or may require a vertical and horizontal extension. Dr Belt can show you in detail the type of procedure your require.
-
What are the causes of excess male breast tissue?
There are numerous causes of excess male breast tissue. In a large number of cases, no cause is found. A full screen is performed to exclude any of the underlying causes. If a cause is found this is obviously treated before any surgery is performed.
-
What are the complications of the procedure?
The risks will be discussed with you in detail before you consent to the operation. The risks can be broken down into general risks associated with any operation, and those specific to gynaecomastia surgery.
General operative risks include anaesthetic complications, bruising, bleeding, infection, wound breakdown and abnormal scarring.
Specific complications include: changes in sensation of the nipple and breast skin, asymmetry, over and under-resection, contour irregularities, loose skin and skin, fat or nipple necrosis (loss).
-
What are the costs involved?
- Dr Belt’s surgical fee
- Assistant’s fee
- Theatre fee / day bed, and overnight bed if not a day case
- Specialist anaesthetists fee
- Costs of compression garment
Rebates are available through both Medicare and Private Health Funds.
Please contact Dr. Belt’s rooms and his staff can answer any questions you may have. A personalised quote and information can be sent to you regarding your procedure.
-
What happens after the operation?
This surgery can performed as a day case procedure. Drains are not normally used. You will be given a prescription for strong painkillers upon discharge from the hospital. You will be advised to wear a compression garment for the first six weeks (day and night). I recommend that you plan a very quiet week immediately after your surgery and avoid driving for 2 weeks and vigorous exercise for 6 weeks.
The stitches are dissolvable and therefore don’t need removing. You will be seen regularly after the operation at one week, two weeks, six weeks and six and 12 months.